Diagnosing & Treating Obstructive Sleep Apnea

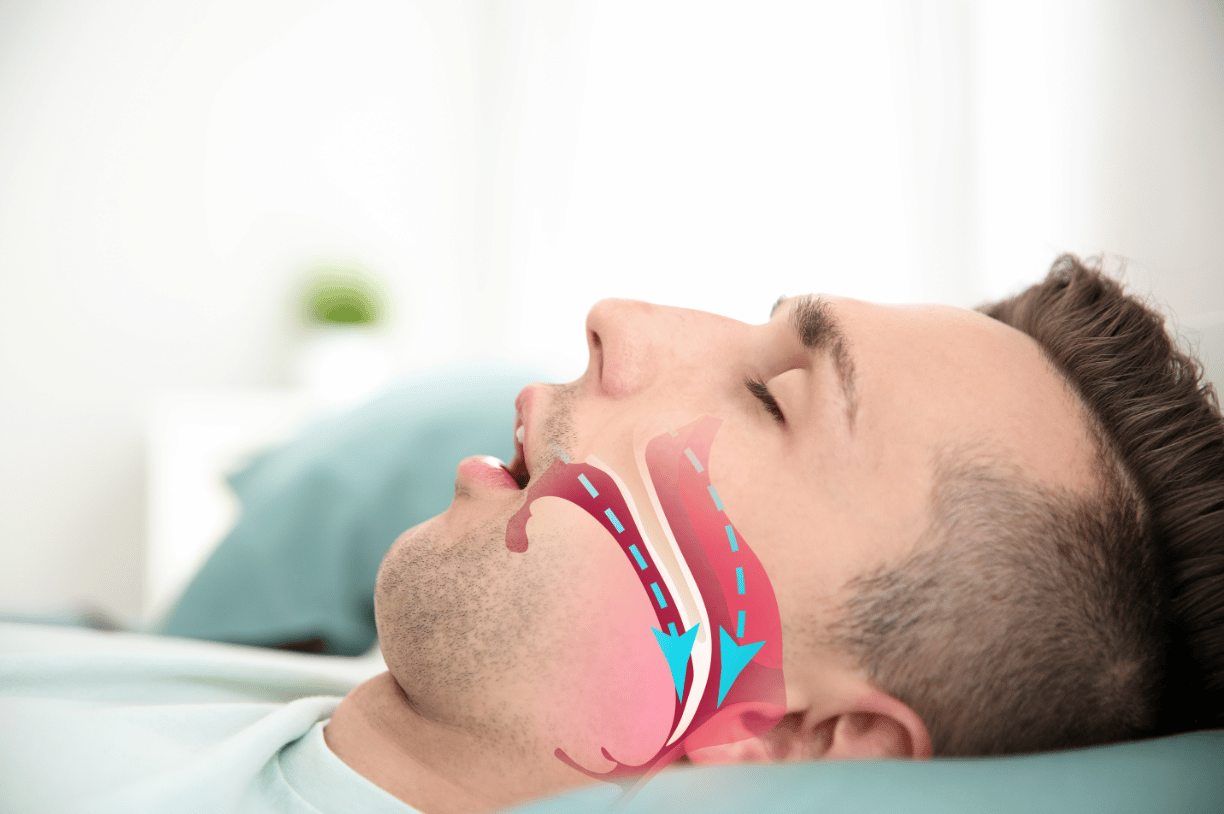
Do you have obstructive sleep apnea (OSA)? This potentially serious sleeping disorder causes your breathing to stop and start repeatedly as often as 30 or more times an hour all night long. You might have OSA if you snore loudly, feel drowsy even after sleeping for a full eight hours, or wake up with a sore throat, dry mouth, or headache. Fortunately, options are available for treating obstructive sleep apnea. You just need the right diagnosis and an effective treatment method.
Diagnosing Obstructive Sleep Apnea
Many different health problems can cause symptoms similar to OSA. After all, not everyone who snores has sleep apnea. Everything from your mouth and nasal cavity anatomy to sleep position and alcohol consumption can lead to snoring.
Other sleep disorders can also cause excessive daytime sleepiness, including insomnia (difficulty falling asleep), narcolepsy (falling asleep suddenly during the day), and restless leg syndrome.
There are even multiple types of sleep apnea. While obstructive sleep apnea stems from overly relaxed throat muscles, central sleep apnea occurs when the brain fails to send proper signals to the muscles that control breathing. When someone has both obstructive and central sleep apnea, the condition is known as complex or mixed sleep apnea.
Each type of sleep apnea calls for a different treatment, so it’s important to diagnose the condition correctly. There are two primary tests for diagnosing OSA: polysomnography and a home sleep apnea test.
Polysomnography is a sleep study conducted in a lab. You are hooked up to equipment that monitors your heart, lungs, brain, breathing patterns, limb movements, and blood oxygen levels while you sleep. Polysomnography is useful for diagnosing obstructive sleep apnea and ruling out other sleep disorders.

A home sleep apnea test provides your doctor with information similar to a polysomnography test, but you get to sleep in the comfort of your own home.
Ask your doctor about these tests if you ever snore loudly enough to disturb your partner, wake up gasping for air, or feel excessively tired during the day. In some cases, your doctor may refer you to an ear, nose, and throat specialist to determine if your sleep apnea could be wholly or partly caused by an anatomic blockage in your nose or throat.
Treating Obstructive Sleep Apnea
Once you have a formal diagnosis, treatment for obstructive sleep apnea can begin.
Lifestyle changes
If you have a mild case of OSA, lifestyle changes may be sufficient to get your symptoms under control. Your doctor may recommend the following:
Lose weight and exercise regularly
Limit your alcohol consumption
Quit smoking
Avoid sleeping on your back
Use nasal decongestant
Avoid taking sleeping pills
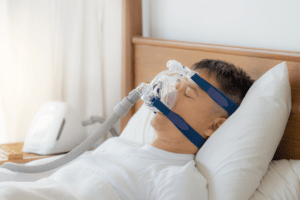
Continuous positive airway pressure (CPAP) machine
When lifestyle changes aren’t enough, consider treating obstructive sleep apnea with other methods. Your doctor may recommend a continuous positive airway pressure (CPAP) machine. This involves wearing a face mask hooked up to a device beside your bed. It delivers constant air pressure to keep your throat open while you sleep.
 Sleep apnea oral device
Sleep apnea oral device
While CPAP is the most commonly prescribed method for treating obstructive sleep apnea, many people find the mask burdensome. It may prevent you from getting comfortable enough to fall asleep, and the noise of the machine might keep you awake.
If you have mild to moderate OSA, you may qualify for another option called a sleep apnea oral device. This popular alternative to CPAP involves wearing a custom-made mouth device that holds your jaw forward slightly, preventing your tongue and other soft tissues from blocking your airway.
Many types of sleep apnea oral devices are available today, but Dr. Ania recommends the MicrO2 Sleep Device. Made from control-cured PMMA, this appliance is more durable, precise, and predictable than other oral devices. It’s also more streamlined for a comfortable, retainer-like fit that makes you more inclined to wear it every night.
Surgery
You should only consider surgical intervention if severe sleep apnea drastically affects your quality of life, and you have attempted other non-invasive options first without success. Uvulopalatopharyngoplasty (UPPP)—the standard surgical procedure for treating obstructive sleep apnea—involves removing some of the soft tissue from the back of your throat. Other surgical options include implants, jaw surgery, and tracheostomy.
Begin Sleep Apnea Treatment Today
After attempting to improve your sleep apnea with lifestyle changes, the next best option may be to try a sleep apnea oral device. Dr. Ania administers home sleep tests and creates custom-made oral sleep apnea devices to change the lives of our patients for the better.
If you still have questions, schedule an appointment with our Boulder dentist by calling 303-443-0998. We look forward to helping you achieve a more restful sleep than you’ve had in years!


